The Doctor Is In!
Welcome to a new feature from PREG where our doctors weigh in on a variety of fertility-related issues designed just for you!

Reproductive Endocrinologist & Partner at PREG.
Aggressive Treatment & Financial Aspects
Dr. Payne, what is aggressive fertility treatment and at what point do you consider it?
Aggressive fertility treatment would be taking a proactive approach in both evaluation and treatment of infertility in such a manner to rapidly progress form less successful (lower probability of conception) to more successful treatments like In vitro fertilization (IVF) with ICSI (injection of one sperm into mature one egg) with possible pre-implantation testing (PGT) an embryo biopsy to determine which embryos are genetically normal before transfer. More aggressive treatments which typically will cost more to do, but have a higher likelihood of achieving pregnancy, may save the patient money in the long run, if less successful treatments are attempted first and do not result in a pregnancy. In general, women that would benefit for a more aggressive approach (IVF/ICSI) might be women over 35 years old, women under 35 who have tried less aggressive treatments, and other issues such as diminished ovarian reserve (low egg numbers), severe male factor with low sperm counts, tubal factor with blocked fallopian tubes, and women with recurrent pregnancy losses. If women have excellent insurance benefits that include IVF, they might consider an aggressive approach initially. In fact, some insurance carriers recommend that their patients start with IVF because the success is so much higher than any other treatment available.
Financial considerations are a big part of fertility treatment, aren’t they?
Many patients think that fertility treatments are out of reach financially, and while they can be expensive, my staff is trained to help maximize benefits and provide information on various savings programs to help make the treatments affordable to all patients.
Can you elaborate on the financial options and plans?
Patient with insurance coverage for infertility treatments will be able to meet with PREG’s financial counselors to learn of their benefits and costs. For patients without insurance coverage for IVF, we have many different options. Full IVF/ICSI (traditional IVF) is the option with the highest success and is required when severe male factor is present or embryo testing is desired, but usually will cost more if no insurance coverage is available.

What are the criteria for considering moving onto an aggressive fertility treatment plan?
There are many reasons to consider moving to an aggressive fertility treatment plan including women over 35 years old, women under 35 who have tried less aggressive treatments and been unsuccessful, diminished ovarian reserve (low egg numbers), severe male factor with low sperm counts, tubal factor with blocked fallopian tubes, and women with recurrent pregnancy losses.
Infertility effects about 10-15% of the reproductive age population or about one in seven couples and well as all same sex couples or single individuals desiring a family. The definition of infertility is women who have had one year of unprotected intercourse without pregnancy as well as women that are over 35 and have been pregnant in the past but are not getting pregnant after six months of trying. We would take a multifaceted approach and look at many factors over one month or menstrual cycle including ovarian reserve testing through labs and ultrasound, fallopian tube and uterine cavity evaluation by hysterosalpingogram (HSG) or saline sonohysterogram (SIS), and semen analysis. Then we meet to review and talk about the different options and review the UNIVFY report for IVF success.
At the follow-up, we try to tailor each patient’s treatment based on the findings in that workup. In general IVF with ICSI is the option that gives them the highest opportunity for success and the fastest way to achieve pregnancy, but it may not be necessary for many women to conceive. Many women could be candidates for lesser treatments like oral fertility medications, ultrasound monitoring, timed intercourse, or intrauterine inseminations. injections to force ovulation to occur.
And what happens from there?
If their evaluation was seemed to show no clear reason for the infertility, otherwise known as unexplained infertility, which happens about 15-20% of the time, then and all the treatment options would be available to them. We could start with ovulation induction, ultrasound monitoring, and a trigger shot to force ovulation within a 36-hour window with timed intercourse for a couple of cycles. Then we will follow up to discuss if we continue with the timed method again, or become more aggressive by adding Intrauterine inseminations which should increase the chance of conception. After a couple of IUI’s, we would meet again and talk about moving on to IVF. The odds of conception each month start to decrease after three to four attempts for each different type of treatment.
What is the biggest factor?
The woman’s age is the most important factor in her natural monthly conception rate, and it is also the biggest factor in success rates with our fertility treatments including timed intercourse, insemination, or IVF. Natural conception rates decline with maternal age and the same time as miscarriage rates increase due maternal age and to the ovarian reserve diminishing. A woman has 5-7 million eggs/follicles in her ovaries around the fifth month of gestation during her mother’s pregnancy. This egg number decreased to two million by birth and is around 500,000 eggs by the time she starts ovulating, so time is critical.
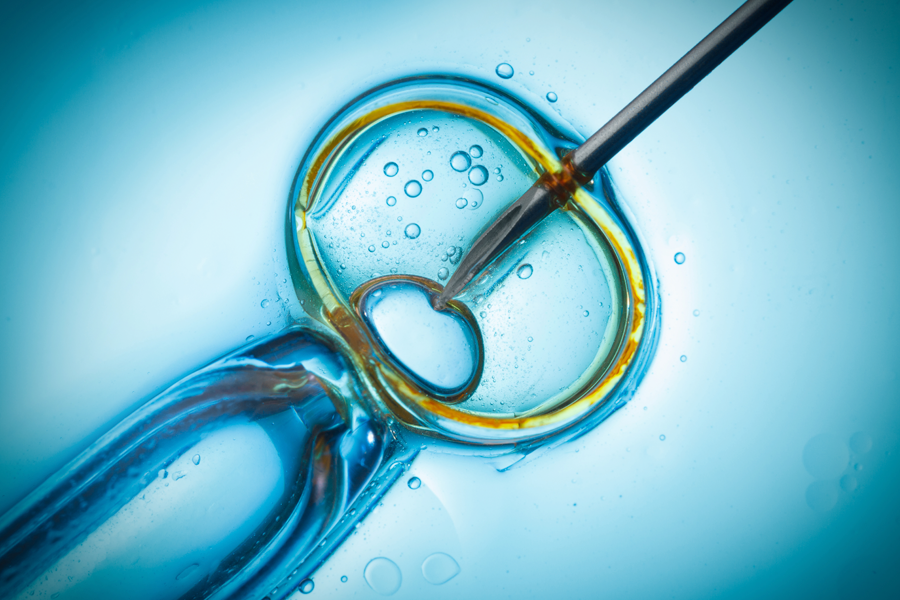
Through IVF, because the eggs and sperm are brought together and fertilization occurs in the lab, we have the ability to observe embryos under a microscope and see how they are progressing over a 6-day period. Using a grading system, we see how they look under a microscope and judge them by certain criteria. Then we can select the embryos which have the most optimal chance for pregnancy. Through IVF we can perform pre-implantation testing (PGT-A). We can biopsy embryos safely removing a 4-6 cells from the portion of the embryo that will form the placenta.
The biopsied embryo is frozen and we send the few cells off to a lab that can test the cells for both aneuploidy (genetically abnormal make-up that is usually incompatible with life) and for single gene mutations (PGT-M) if the couple is found to be at risk of having a child with a certain disease by carrier screening. Some of the common gene mutations like carriers of cystic fibrosis, sickle cell, Duchenne muscular dystrophy and many other genetic abnormalities can be found this way. We can then select an embryo that is euploid (normal chromosomes) and not affected by the disease that the couple carried. At PREG we follow practice guidelines for embryo transfer that were developed to try to optimize pregnancy success while minimizing risk of multiple gestations (twins or more). We try to perform single embryo transfers as much as possible. In theory, transferring one genetically normal embryo at a time should allow for a high likelihood of pregnancy and reduce the risk for a miscarriage over embryos that have not been tested.

PREG has offices in Greenville, Spartanburg, Asheville, and Columbia. We offer highly personalized fertility care and management. Dr. Payne is based at the Greenville, SC, office. For more information on reproductive options call, or contact us today at 866.725.7734, or online at http://www.pregonline.com/contact-us.php
Dr. John Frederick Payne, MD
Reproductive Endocrinologist, Partner,
and Third-Party Reproduction Director at PREG