 Dr. John E. Nichols, Jr., MD
Dr. John E. Nichols, Jr., MD
Reproductive Endocrinologist and Infertility Specialist
PREG Founder
Medical & Laboratory Director
Dr. Nichols answers questions about “Egg Retrieval During IVF”
What is egg retrieval in IVF?
The process of In Vitro Fertilization (IVF), which is an aggressive and thankfully very successful fertility treatment, is comprised of several steps. One of the first steps we begin with is called ovarian hyper-stimulation where the woman takes injectable fertility medications for around 10-12 days to stimulate the ovaries to make multiple follicles (fluid-filled sacs containing eggs). We try to get these follicles to grow to a certain size (around 18 to 20 mm) so that when we go in to retrieve the eggs, we can get mature eggs that have the highest chance to fertilize and then allow them to develop into embryos called blastocysts. We can then transfer the blastocyst (usually one!!) back into the patient’s uterus to give her the best chance for pregnancy success.
Once the ovarian follicles are ready, we set up to perform an egg retrieval procedure which is done in our fully accredited operating rooms (ORs) that we have available in our Greenville, Columbia, and Lowcountry offices. The patient is given an IV in her arm and then we use quick-acting medications to sedate them, given by a CRNA (Certified Registered Nurse Anesthetist), and put them into a “twilight sleep” in which the patient is not totally asleep, is still able to breathe on their own and we can gently awaken them if needed but it’s enough sedation for her to relax without feeling the egg retrieval process.

How long does it take?
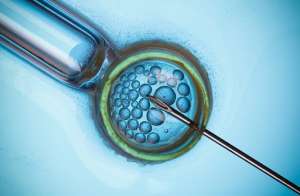
What are you trying to accomplish during this procedure?
So, the whole idea of stimulation of the ovaries during those 10 – 12 days is to try and push the ovaries to develop as many follicles/eggs as we can. We then want to get the eggs to the lab where the hard work begins. Fertilization then begins with either putting sperm with the eggs or actual placement of a single normal sperm into the egg (ICSI, Intracytoplasmic Sperm Injection). Once the egg is successfully fertilized then we allow the embryos to grow in the lab for 5-6 days to get to the blastocyst stage which is a highly developed embryo. It is at this point then we can consider an embryo transfer to place the blastocyst into the patient’s uterus (fresh embryo transfer) or can freeze all the blasts and then transfer back into the uterus at later date (frozen embryo transfer). In addition, at the blastocyst stage, an embryo biopsy (PGT, Preimplantation Genetic Testing) can be performed to remove several cells from the embryo to be sent off for chromosomal analysis to ensure that the embryo is genetically normal. In addition, if a patient or couple has some type of genetic disease(s) we can screen the embryos for the specific disease and then only transfer the embryos that will not be affected by the disease.
How do you do embryo transfer or what is the timetable from that point?
It depends on whether we are doing a fresh transfer or a frozen transfer. A fresh transfer can be done within five days of the retrieval. In the cases that we are doing genetic testing, we cannot do a fresh transfer since the cells removed from the embryo will be sent to a specialized testing lab and can take up to two weeks to get the results back. So, we would then freeze all the embryos and then transfer back at later date (generally in 4-6 weeks) the appropriate or normal embryo. Frozen embryo transfer may also be recommended instead of a fresh transfer if the patient’s hormone levels during the IVF stimulation are too high since those high levels could affect how well the embryo may implant in a fresh cycle.
To get the uterus ready for a frozen embryo transfer is much easier since only using lower doses of hormones to prepare the uterine lining (endometrium) and then transferring the embryo at an appropriate time. We use a small embryo transfer catheter which we pass through the cervix, and with the use of an abdominal ultrasound probe to visualize, place the embryo near the top of the uterine cavity to give it the best chance for success. The patient can get up immediately after embryo transfer (no bed rest needed), but we do recommend limited activities (no vigorous exercise or major physical work) for that day and then back to regular activities the next day.

PREG has offices in Greenville, Spartanburg, Asheville, Columbia, and Lowcountry. Our surgery centers are located in Greenville, Columbia, and Lowcountry. We offer highly personalized fertility care and management. Dr. Nichols is based in Greenville, SC, office. For more information on reproductive options call, or contact us today at 866.725.7734, or online at http://www.pregonline.com/contact-us.php



 Dr. John E. Nichols, Jr., MD
Dr. John E. Nichols, Jr., MD
